A look at maternal death rate increase and its implications
August 27, 2017 / in Media & Awards
Printed by the New Hampshire Union Leader on August 27, 2017
Article written by Dr. Caroline Scoones and Dr. Emily Amarosa of Harbour Women’s Health
A worrisome trend has recently been highlighted regarding maternal health in the United States of America. Despite being a global powerhouse and spending $3 trillion on healthcare each year, the United States is lagging significantly behind other developed nations in maternal mortality rate. More disheartening, this rate has been steadily increasing since the early 2000s while other nations have had a steady decrease during the same period.

Dr. Caroline Scoones

Dr. Emily Amarosa
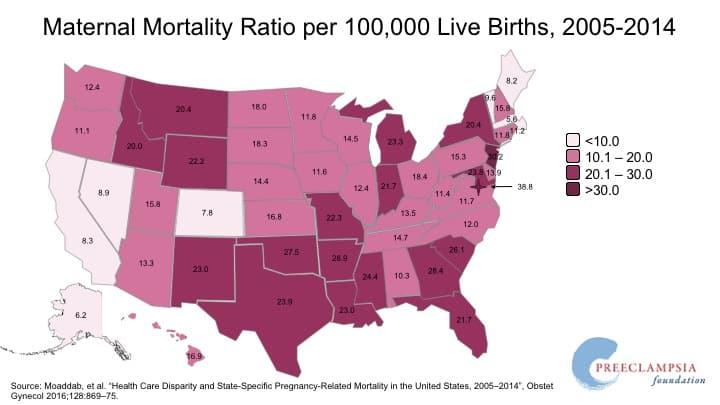
According to the accompanying map provided by the Preeclampsia Foundation, the maternal mortality ratio per 100,000 live births was 15.8 in New Hampshire between 2005 and 2014.
There is no one easy answer to why this increase is taking place. However, experts agree there are many contributing factors.
Our maternal population is on average older and with more medical problems than most nations. There are also large disparities in access to adequate care amongst women of different races and socio-economic backgrounds. Finally, we have a healthcare system that is at times complex and difficult to navigate.
Medical risk factors
The medical risk factors that women bring into pregnancy highlight an area of opportunity to help address this rising mortality. Increased rates of diabetes, heart disease, high blood pressure and obesity are all associated with poor maternal outcomes. When you consider that at least 50 percent of pregnancies in America are unplanned, this means that many women have not adequately controlled these medical risk factors prior to conception. This emphasizes the need for safe and effective contraception for women who are not ready to become pregnant and pre-conceptual counseling for women who are planning pregnancy. Regardless, there is a need for early initiation of prenatal care to identify and treat conditions dangerous to pregnancy and delivery.
Responding to complications
From 2011-13, leading causes of maternal mortality in America included cardiovascular and other heart disease, infection or sepsis, hemorrhage, pulmonary embolism, hypertensive disorders of pregnancy and stroke. Receiving care within an institution that can respond to emerging medical complications and by providers who can respond to urgent issues during and after delivery helps to reduce these risks. Valuable ancillary services include a well-equipped blood bank, readily-available anesthesiologists, cardiologists, intensive care physicians, and infectious disease specialists, and a labor and delivery staff familiar with early and subtle symptoms of potentially life-threatening events. For example, our labor and delivery unit at Portsmouth Regional Hospital performs drills to help sustain a coordinated response from nursing staff, physicians and ancillary services to be prepared for these types of events.
Access to care
Finally, access to care is a huge contributing factor in prevention, early detection and prompt treatment of pregnancy complications.
The Affordable Healthcare Act has helped improve access to care greatly but huge deficits remain. Texas was recently identified as the state with the highest maternal mortality rate and one of the states with very poor access to care. In contrast, California offers an expanded Medicaid and unified health care system and is one of the only states that has decreased maternal mortality rate during this same time period.
Although the rate of maternal mortality in America is relatively high, the absolute risk remains quite low and most pregnancies have healthy outcomes for both mother and baby. This spotlight on maternal mortality has also sparked very positive results, including new bipartisan legislation to support states’ attempts to reduce this rate and improve maternal health.
Dr. Caroline Scoones and Dr. Emily Amarosa are OB/GYNs at Harbour Women’s Health located in Portsmouth, and practice at Portsmouth Regional Hospital, which offers a Level 2 Trauma Center with the ancillary services referenced above.
Read more on the New Hampshire Union Leader website